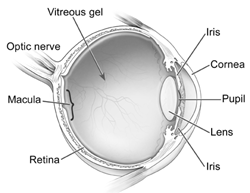
What is diabetic eye disease?
Diabetic eye disease refers to a group of eye problems that people
with diabetes may face as a complication of diabetes. All can cause
severe vision loss or even blindness.
Diabetic eye disease may include:
- Diabetic retinopathy—damage to the blood vessels in the retina.
- Cataract—clouding of the eye’s lens. Cataracts develop at an earlier age in people with diabetes.
- Glaucoma—increase
in fluid pressure inside the eye that leads to optic nerve damage and
loss of vision. A person with diabetes is nearly twice as likely to get
glaucoma as other adults.
What is diabetic retinopathy?
Diabetic retinopathy is the most common diabetic eye disease and a
leading cause of blindness in American adults. It is caused by changes
in the blood vessels of the retina.
In some people with diabetic retinopathy, blood vessels may swell and
leak fluid. In other people, abnormal new blood vessels grow on the
surface of the retina. The retina is the light-sensitive tissue at the
back of the eye. A healthy retina is necessary for good vision.
If you have diabetic retinopathy, at first you may not notice changes
to your vision. But over time, diabetic retinopathy can get worse and
cause vision loss. Diabetic retinopathy usually affects both eyes.
What are the stages of diabetic retinopathy?
Diabetic retinopathy has four stages:
- Mild Nonproliferative Retinopathy. At this earliest stage, microaneurysms occur. They are small areas of balloon-like swelling in the retina’s tiny blood vessels.
- Moderate Nonproliferative Retinopathy. As the disease progresses, some blood vessels that nourish the retina are blocked.
- Severe Nonproliferative Retinopathy. Many more
blood vessels are blocked, depriving several areas of the retina with
their blood supply. These areas of the retina send signals to the body
to grow new blood vessels for nourishment.
- Proliferative Retinopathy. At this advanced stage,
the signals sent by the retina for nourishment trigger the growth of
new blood vessels. This condition is called proliferative retinopathy.
These new blood vessels are abnormal and fragile. They grow along the
retina and along the surface of the clear, vitreous gel that fills the
inside of the eye. By themselves, these blood vessels do not cause
symptoms or vision loss. However, they have thin, fragile walls. If they
leak blood, severe vision loss and even blindness can result.
Causes and Risk Factors
How does diabetic retinopathy cause vision loss?
Blood vessels damaged from diabetic retinopathy can cause vision loss in two ways:
- Fragile, abnormal blood vessels can develop and leak blood into the center of the eye, blurring vision. This is proliferative retinopathy and is the fourth and most advanced stage of the disease.
- Fluid can leak into the center of the macula, the part of the eye
where sharp, straight-ahead vision occurs. The fluid makes the macula
swell, blurring vision. This condition is called macular edema.
It can occur at any stage of diabetic retinopathy, although it is more
likely to occur as the disease progresses. About half of the people with
proliferative retinopathy also have macular edema.
Normal Vision and the same scene viewed by a person with diabetic retinopathy.
Normal vision

Same scene viewed by a person with diabetic retinopathy
Who is at risk for diabetic retinopathy?
All people with diabetes–both type 1 and type 2–are at risk. That’s
why everyone with diabetes should get a comprehensive dilated eye exam
at least once a year. The longer someone has diabetes, the more likely
he or she will get diabetic retinopathy. Between 40 to 45 percent of
Americans diagnosed with diabetes have some stage of diabetic
retinopathy. If you have diabetic retinopathy, your doctor can recommend
treatment to help prevent its progression.
During pregnancy, diabetic retinopathy may be a problem for women
with diabetes. To protect vision, every pregnant woman with diabetes
should have a comprehensive dilated eye exam as soon as possible. Your
doctor may recommend additional exams during your pregnancy.
What can I do to protect my vision?
If you have diabetes get a comprehensive dilated eye exam at least once a year and remember:
- Proliferative retinopathy can develop without symptoms. At this advanced stage, you are at high risk for vision loss.
- Macular edema can develop without symptoms at any of the four stages of diabetic retinopathy.
- You can develop both proliferative retinopathy and macular edema
and still see fine. However, you are at high risk for vision loss.
- Your eye care professional can tell if you have macular edema or any
stage of diabetic retinopathy. Whether or not you have symptoms, early
detection and timely treatment can prevent vision loss.
If you have diabetic retinopathy, you may need an eye exam more
often. People with proliferative retinopathy can reduce their risk of
blindness by 95 percent with timely treatment and appropriate
follow-up care.
The Diabetes Control and Complications Trial (DCCT) showed that
better control of blood sugar levels slows the onset and progression of
retinopathy. The people with diabetes who kept their blood sugar levels
as close to normal as possible also had much less kidney and nerve
disease. Better control also reduces the need for sight-saving
laser surgery.
This level of blood sugar control may not be best for everyone,
including some elderly patients, children under age 13, or people with
heart disease. Be sure to ask your doctor if such a control program is
right for you.
Other studies have shown that controlling elevated blood pressure and
cholesterol can reduce the risk of vision loss. Controlling these will
help your overall health as well as help protect your vision.
Symptoms and Detection
Does diabetic retinopathy have any symptoms?
Often there are no symptoms in the early stages of the disease, nor is there any pain.
Don’t wait for symptoms. Be sure to have a comprehensive dilated eye exam at least once a year.
Blurred vision may occur when the macula—the part of the retina that
provides sharp central vision—swells from leaking fluid. This condition
is called macular edema.
If new blood vessels grow on the surface of the retina, they can bleed into the eye and block vision.
What are the symptoms of proliferative retinopathy if bleeding occurs?
At first, you will see a few specks of blood, or spots, “floating” in
your vision. If spots occur, see your eye care professional as soon as
possible. You may need treatment before more serious bleeding occurs.
Hemorrhages tend to happen more than once, often during sleep.
Sometimes, without treatment, the spots clear, and you will see
better. However, bleeding can reoccur and cause severely blurred vision.
You need to be examined by your eye care professional at the first sign
of blurred vision, before more bleeding occurs.
If left untreated, proliferative retinopathy can cause severe vision
loss and even blindness. Also, the earlier you receive treatment, the
more likely treatment will be effective.
How are diabetic retinopathy and macular edema detected?
Diabetic retinopathy and macular edema are detected during a comprehensive eye exam that includes:
- Visual acuity test. This eye chart test measures how well you see at various distances.
- Dilated eye exam. Drops are placed in your eyes to
widen, or dilate, the pupils. This allows the eye care professional to
see more of the inside of your eyes to check for signs of the disease.
Your eye care professional uses a special magnifying lens to examine
your retina and optic nerve for signs of damage and other eye problems.
After the exam, your close-up vision may remain blurred for
several hours.
- Tonometry. An instrument measures the pressure inside the eye. Numbing drops may be applied to your eye for this test.
Your eye care professional checks your retina for early signs of the disease, including:
- Leaking blood vessels.
- Retinal swelling (macular edema).
- Pale, fatty deposits on the retina–signs of leaking blood vessels.
- Damaged nerve tissue.
- Any changes to the blood vessels.
If your eye care professional believes you need treatment for macular edema, he or she may suggest a
fluorescein angiogram.
In this test, a special dye is injected into your arm. Pictures are
taken as the dye passes through the blood vessels in your retina. The
test allows your eye care professional to identify any leaking blood
vessels and recommend treatment.
Treatment
How is diabetic retinopathy treated?
During the first three stages of diabetic retinopathy, no treatment
is needed, unless you have macular edema. To prevent progression of
diabetic retinopathy, people with diabetes should control their levels
of blood sugar, blood pressure, and blood cholesterol.
Proliferative retinopathy is treated with laser surgery. This
procedure is called scatter laser treatment. Scatter laser treatment
helps to shrink the abnormal blood vessels. Your doctor places 1,000 to
2,000 laser burns in the areas of the retina away from the macula,
causing the abnormal blood vessels to shrink. Because a high number of
laser burns are necessary, two or more sessions usually are required to
complete treatment. Although you may notice some loss of your side
vision, scatter laser treatment can save the rest of your sight. Scatter
laser treatment may slightly reduce your color vision and night vision.
Scatter laser treatment works better before the fragile, new blood
vessels have started to bleed. That is why it is important to have
regular, comprehensive dilated eye exams. Even if bleeding has started,
scatter laser treatment may still be possible, depending on the amount
of bleeding.
If the bleeding is severe, you may need a surgical procedure called a
vitrectomy. During a vitrectomy, blood is removed from the center of
your eye.
How is a macular edema treated?
Macular edema is treated with laser surgery. This procedure is called
focal laser treatment. Your doctor places up to several hundred small
laser burns in the areas of retinal leakage surrounding the macula.
These burns slow the leakage of fluid and reduce the amount of fluid in
the retina. The surgery is usually completed in one session. Further
treatment may be needed.
A patient may need focal laser surgery more than once to control the
leaking fluid. If you have macular edema in both eyes and require laser
surgery, generally only one eye will be treated at a time, usually
several weeks apart.
Focal laser treatment stabilizes vision. In fact, focal laser
treatment reduces the risk of vision loss by 50 percent. In a small
number of cases, if vision is lost, it can be improved. Contact your eye
care professional if you have vision loss.
NEI research found that prompt treatment of macular edema with the
drug Lucentis, with or without laser treatment, resulted in better
vision than laser treatment alone or steroid injections. When injected
into the eye, Lucentis, and two other similar drugs, Avastin or Aylea,
reduce fluid leakage and interfere with the growth of new blood vessels
in the retina. NEI is sponsoring a study comparing the three drugs, in
the mean time, your doctor will help you decide what is best for you.
What happens during laser treatment?
Both focal and scatter laser treatment are performed in your doctor’s
office or eye clinic. Before the surgery, your doctor will dilate your
pupil and apply drops to numb the eye. The area behind your eye also may
be numbed to prevent discomfort.
The lights in the office will be dim. As you sit facing the laser
machine, your doctor will hold a special lens to your eye. During the
procedure, you may see flashes of light. These flashes eventually may
create a stinging sensation that can be uncomfortable.
You will need someone to drive you home after surgery. Because your
pupil will remain dilated for a few hours, you should bring a pair
of sunglasses.
For the rest of the day, your vision will probably be a little blurry. If your eye hurts, your doctor can suggest treatment.
Laser surgery and appropriate follow-up care can reduce the risk of
blindness by 90 percent. However, laser surgery often cannot restore
vision that has already been lost. That is why finding diabetic
retinopathy early is the best way to prevent vision loss.
What is a vitrectomy?
If you have a lot of blood in the center of the eye (vitreous gel),
you may need a vitrectomy to restore your sight. If you need
vitrectomies in both eyes, they are usually done several weeks apart.
A vitrectomy is performed under either local or general anesthesia.
Your doctor makes a tiny incision in your eye. Next, a small instrument
is used to remove the vitreous gel that is clouded with blood. The
vitreous gel is replaced with a salt solution. Because the vitreous gel
is mostly water, you will notice no change between the salt solution and
the original vitreous gel.
You will probably be able to return home after the vitrectomy. Some
people stay in the hospital overnight. Your eye will be red and
sensitive. You will need to wear an eye patch for a few days or weeks to
protect your eye. You also will need to use medicated eyedrops to
protect against infection.
Are scatter laser treatment and vitrectomy effective in treating proliferative retinopathy?
Yes. Both treatments are very effective in reducing vision loss.
People with proliferative retinopathy have less than a five percent
chance of becoming blind within five years when they get timely and
appropriate treatment. Although both treatments have high success rates,
they do
not cure diabetic retinopathy.
Once you have proliferative retinopathy, you always will be at risk
for new bleeding. You may need treatment more than once to protect
your sight.
What can I do if I already have lost some vision from diabetic retinopathy?
If you have lost some sight from diabetic retinopathy, ask your eye
care professional about low vision services and devices that may help
you make the most of your remaining vision. Ask for a referral to a
specialist in low vision. Many community organizations and agencies
offer information about low vision counseling, training, and other
special services for people with visual impairments. A nearby school of
medicine or optometry may provide low vision services